
From April to December 2020, we tracked the nutritional status, risk of sarcopenia and nutritional complaints of all patients with COVID-19 in four Dutch hospitals: Amsterdam UMC, Zuyderland MC and Franciscus & Vlietland hospital. This was measured during hospitalization and after discharge by 18 dieticians in the hospitals and by 64 dieticians outside the hospital. In other words, real teamwork!
“Prevention, timely recognition and treatment of malnutrition should be standard care for patients with COVID-19”
The results were published in Clinical Nutrition ESPEN. On this page, you can download the article, watch the video, read more about the results and recommendations are download the booklet.


Video
Video URL: https://www.youtube.com/watch?v=9oO32H4NsSM
How big is the problem?

40-50% of patients with COVID-19 in the hospital are malnourished. 2-5
Intensive care patients lose a lot of muscle mass. This can be as high as 1 kg of muscle mass loss per day. 6,7
Individuals at high risk for a severe course of COVID-19 are also at high risk for malnutrition and sarcopenia1
- Older persons8
- Intensive care patients3
- Chronically ill patients1
Malnutrition and sarcopenia have implications for disease progression and recovery4,8,11-13
- Decreased functionality due to loss of muscle mass and strength.
- Increased risk of complications.
- A longer recovery period.
- Greater risk of death.
- Obese individuals7,9
Why do patients with COVID-19 have a high risk of malnutrition and sarcopenia?
- Almost all patients have nutritional complaints that make eating difficult.3
- Increased energy consumption due to high disease activity.6,10
- High muscle mass breakdown and low muscle mass gain due to bed rest, insulin resistance, and high disease activity.6,10
Results
Despite 67% being overweight, 35% of patients were malnourished at admission to the hospital. Almost all patients had one or more nutritional complaints. Of these complaints, decreased appetite, feeling of being full, altered taste, and loss of taste were the most common nutritional complaints (see figure).
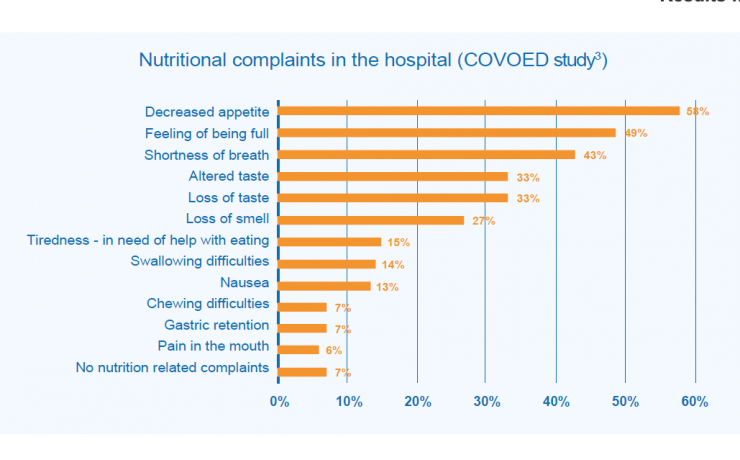
In hospitals
- There should be early screening for malnutrition; involve the dietitian early in treatment.
- Patients in the hospital with an inadequate nutritional intake should switch to enteral or possibly parenteral nutrition in a timely manner. The loss of muscle mass is too rapid and severe to wait long to do so.
- Patients in intensive care have high nutritional requirements. Choosing the amount and type of tube feeding should be tailored per patient.
- After ventilation, many patients develop swallowing problems. Screening and early treatment of swallowing problems can prevent further deterioration of nutritional status.
- Almost all patients who have been in the intensive care unit require dietetic care after discharge from the hospital. Transfer nutritional treatment to a dietitian in primary care or the rehabilitation center.
In the home situation
- For the COVID-19 patient with (risk of) malnutrition, nutritional treatment must be continued by the dietitian after discharge from the hospital. Physical therapy, exercise therapy, occupational therapy and speech therapy should also be considered.
- In case of swallowing problems, texture adjustments to the diet, after consulting a speech therapist, should be considered.
- Patients and caregivers should be informed about the importance of following nutritional treatment, self-screening of nutritional risks, and indications of when to contact caregivers.
- Patients who have been in intensive care for a long time are at very high risk for post ICU syndrome (PICS). Include this in treatment and evaluation.
Literature
- Barazzoni R, et al. Clin Nutr. 2020; 39(6):1631-1638
- Bedock D, et al. Clin Nutr. ESPEN 2020; 40:214-219
- Wierdsma N, et al. Clin Nutr ESPEN 2021
- Allard L, et al. Nutrients 2020; 12(12): 3679
- Wei C, et al. J Clin Biochem Nutr. 2020;67(2):116-121
- Van Zanten A, et al. Crit Care. 2019; 23(1):368
- Gualtieri P, et al. Int J Mol Sci. 2020; 21(13): 467
- Azzolino D, et al. J Nutr Health Aging. 2020;24(7):696-698
- Chiappetta S, et al. Int J Obes (Lond). 2020;44(8):1790-1792
- Whittle J, et al. Critical Care (2020) 24:581
- Belli S, et al. Eur Respir J. 2020;56(4):2002096
- Taboada M, et al. J Infect. 2020;S0163-4453(20)30784-2
- Cederholm T, et al. Clin Nutr. 2019 ;38(1):1-9

Contact Elke for inquiries on Dutch campaign activities and for publishing of your Good Practice on this website.




